
What Is Medical Billing Outsourcing and How Does It Benefit Healthcare Providers?
Medical billing outsourcing is when a healthcare organization contracts a third-party provider to handle its back-end billing, freeing up on-site staff to focus on patient care and administrative duties. This benefits healthcare providers by streamlining Revenue Cycle Management, reducing staffing and overhead costs, and increasing accounts receivable.
Read Time: 9 minutes
Table of Contents
Introduction
Medical billing plays a critical role in the financial health of healthcare organizations, yet it has become increasingly complex as regulations evolve, coding requirements grow more detailed, and administrative demands intensify. Providers are under constant pressure to maintain accuracy, compliance, and timely reimbursements, all while prioritizing patient care. As a result, many healthcare organizations are rethinking traditional in-house billing models and exploring healthcare call center services & outsourcing as a strategic solution.
This guide examines medical billing outsourcing in depth, explaining how it works, its benefits and challenges, cost considerations, and emerging trends shaping the future of healthcare revenue cycle management.
Key takeaways
- Medical billing outsourcing improves efficiency, accuracy, and cash flow by leveraging dedicated experts, advanced technology, and compliance-first processes to reduce errors, speed up reimbursements, and strengthen revenue cycle management.
- The right outsourcing partner mitigates risk while enabling scalability, integrating seamlessly with existing systems, protecting patient data, and scaling resources to meet changing demand.
- Technology-driven innovation is shaping the future of medical billing. AI and advanced analytics are improving accuracy, reducing denials, and delivering deeper insights into financial performance, making outsourcing a strategic advantage heading into 2026.

What is medical billing outsourcing?
Medical billing outsourcing is when a healthcare provider contracts a third-party organization to handle insurance claims and Revenue Cycle Management. External specialists can handle the following key functions to relieve burden on internal employees.
- Coding: Experts can reduce coding errors and ensuing delays, fees, or penalties by interpreting notes and accurately applying standardized codes.
- Claims management: Outsourced teams submit, track, and follow up on insurance claims, identifying problems or delays before they impact cash flow.
- Collections: Medical billing BPOs follow strict compliance regulations to protect patient information while handling payments.
How medical billing outsourcing works
In-house healthcare teams struggle to manage the complexity of medical billing as regulations constantly change and attention is further divided between patient care and administration duties.
Medical billing outsourcing teams, by contrast, are dedicated to the task. They streamline processes to seamlessly handle all steps involved in medical billing.
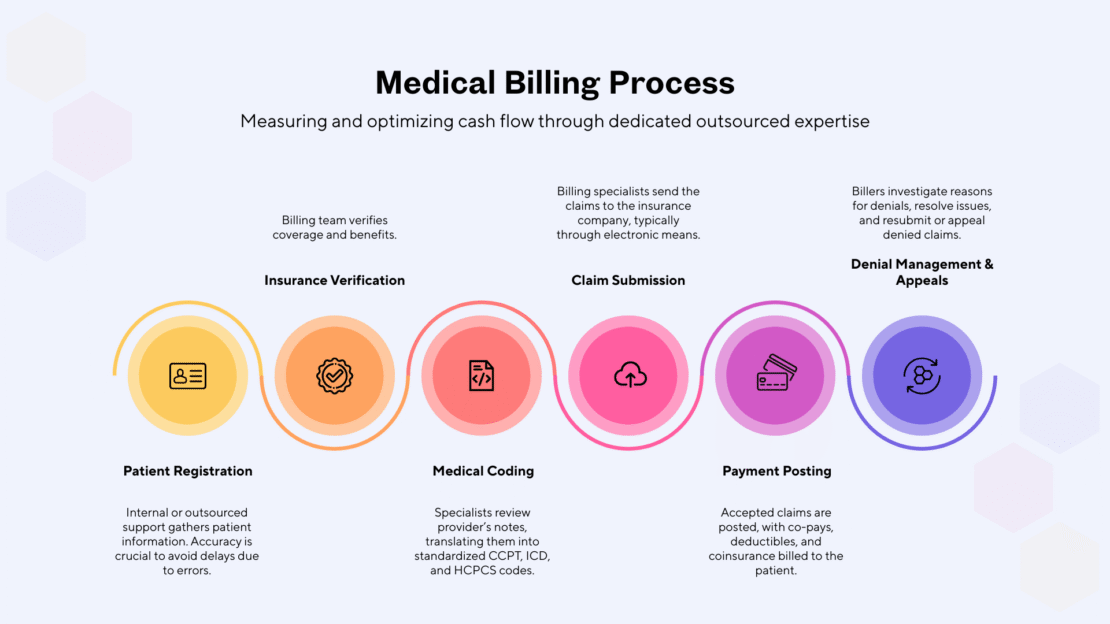
Step 1: Claims submission.
Depending on the outsourcing model, outsourced teams handle all patient intake and registration or work with in-house teams to do so. They then collect and verify insurance and obtain prior authorization to ensure services qualify for payment.
Step 2: Coding.
Outsourcing providers utilize coding experts to translate clinical notes into standardized CPT (Current Procedural Terminology), ICD-10 (International Classification of Diseases), and HCPCS (Healthcare Common Procedure Coding System) codes.
They also review coding to reduce errors that can lead to denials or reduced reimbursements, ensuring patient satisfaction and accurate service. Outsourced medical billing providers should leverage specialized experts and ongoing training to ensure successful coding.
Step 3: Claims follow-up.
Monitoring the status of every claim is essential to accurate and cost-effective medical billing. Outsourced specialists investigate denied claims, resolve issues, and submit appeals with correct information to ensure cash flow.
Benefits of outsourcing medical billing
Medical billing issues can prove costly, putting providers and patients at risk. Outsourcing helps medical practices overcome operational challenges, enabling them to focus on better care and sustainable patient and provider success.
These medical billing outsourcing benefits leave lasting positive impacts on practices of all sizes, increasing revenue and enabling more efficient healthcare.
Cost efficiency: Known for its cost-effectiveness, outsourcing reduces internal staffing and overhead costs while improving cash flow through dedicated expertise.
Accuracy and compliance: Medical billing outsourcing providers streamline processes and increase billing accuracy. High-quality providers are HIPAA compliant and follow strict protocols to ensure data privacy and security.
Faster reimbursements: Proactive medical billing strategies reduce delays and errors common to internal overwhelm, moving claims along the process swiftly and reducing gaps in payments.
Scalability and flexibility: Outsourcing providers leverage ready-to-work experts from global agent pools to efficiently manage demand fluctuations on any timetable without the high costs of internal hiring.
Challenges and risks
While medical billing outsourcing can benefit your practice significantly, working with an external provider can raise concerns to address for an effective partnership.
Data security and HIPAA compliance:
Any external access to your healthcare operations presents a security risk, but expert healthcare service providers follow strict security protocols to protect patient information. High-level encryption, secure frameworks, clear access controls, and strict HIPAA compliance in medical billing outsourcing prevent data breaches and reduce errors in RCM outsourcing.
Communication and control issues:
While outsourcing is meant to relieve overwhelm, some providers can struggle to adjust to the change in responsibilities or lack of oversight into daily medical billing processes. Finding the right fit in culture, work ethic, and communication style and cadence is vital to a beneficial partnership.
Dependence on third-party vendor:
Outsourcing requires aligning not only strategies and culture but also systems and processes. A provider should easily integrate with your Electronic Health Record system for a smooth and secure transition. Transparent practices, communication, and reporting will ensure both parties meaningfully contribute to the goals of the organization.
Want to scale your business?
Global Response has a long track record of success in outsourcing customer service and call center operations. See what our team can do for you!
How to choose the right medical billing outsourcing company
Who you choose to entrust medical billing processes to can affect the success and reputation of your practice. Your partner should align with your goals and standards. Accurately assess your potential options by analyzing these evaluation criteria of medical billing outsourcing companies.
- Experience: Healthcare BPOs should have extensive experience handling medical billing for organizations of your size and scope. Their strategies will target specific challenges with effective, scalable medical billing outsourcing solutions.
- Compliance: The right medical billing provider will operate with a compliance-first mindset to protect your organization and clientele. This boosts not only adherence but also efficiency, cash flow, and satisfaction for a meaningful impact.
- Technology: A medical billing leader will navigate complex challenges using a combination of irreplaceable human experts and advanced technological resources. Streamlined processes and AI-powered live assistance enhance performance while maximizing efficiency.
- Transparency: The right medical billing partner operates with full transparency as a partner dedicated to your immediate and long-term success. Ask about performance metrics tracked, reporting cadence, training programs, and accountability measures to find a partner that aligns with your vision and your values.
Tip: Ask to read case studies to evaluate the results and processes of similar campaigns.

In-house vs outsourced medical billing
Outsourcing should be a strategic decision your practice makes toward scalable success. Determine the effectiveness of third-party medical billing by comparing it with internal capacity to see if it’s the right time to outsource.
In-house medical billing | Outsourced medical billing |
Salaries, benefits, training, and software expenses rise with overwhelm, attrition, errors, and demand surge | Access to dedicated experts reduces overhead costs and maximizes reimbursements |
Direct oversight over processes is constrained by administrative availability | Reduces internal control while leveraging external managers dedicated to improving RCM |
Direct control over compliance adherence requires accurate, flexible resource allocation | Compliance experts keep practices up to date with evolving regulations |
Expanding team size requires significant financial, resource, and time investments | Easily manages scalability needs, growing or shrinking teams on custom timelines and budgets |
Cost of medical billing outsourcing
Outsourcing can be a powerful strategy to level up your operational efficiency and success, making it a cost-effective long-term solution for scalable healthcare practices. But making the switch at the right time will maximize financial gains and growth potential.
Determine if outsourced medical billing is the right fit for your practice financially by finding a partner who takes into account these important factors for a truly custom solution.
- Services provided: Medical billing, Revenue Cycle Management, customer support, or other administrative and back-end work
- Specialty expertise: Coding experts, medical billing specialists, workers who understand nuances between different medical fields
- Agent headcount: Minimums ensure profitability and efficient handling of claim volume. Prices rise with agent headcount while flexible workforce solutions maximize cost-effectiveness year-round.
- Sourcing location: US-based agents are typically the most expensive, with nearshore agents in mid-range and offshore agents being the most affordable.
Pricing models for medical billing outsourcing costs vary depending on the provider. Each provides a cost-effective approach for medical billing outsourcing.
Percentage of Collections: The medical billing company charges a fee based on a percentage of total collections processed, often between 4% and 8%.
- Example: Processing 100,000 claims in a month on a 6% rate will cost $6,000 that month.
Per-Claim Fees: Fees per claim submitted can range from $4 to $10 per claim, depending on complexity and volume.
- This model is an ideal approach to medical billing outsourcing for small practices with fewer claims.
Flat Monthly Fees: Ranging from $500 to $5,000 this model covers all billing stages and takes into account size of the practice and complexity of services.
- This can be particularly effective for companies experiencing predictable volume and claim types.
Hybrid: Hybrid models involve a mix of a percentage of collections with flat fees for services. Simple tasks can come with set fees while percentage-based costs accommodate more complex tasks such as handling denied claims.
- This combines predictability while incentivizing performance.
Trends in medical billing outsourcing for 2026
The medical billing outsourcing market thrives for its adaptability, and it is expected to grow with innovations in technology to keep up with patient and provider needs. Keep track of these medical billing outsourcing trends to stay ahead of the curve with the latest cutting-edge strategies.
AI and automation: Artificial intelligence is revolutionizing healthcare. AI tools improve coding and billing accuracy, which reduces denials and plays a significant role in streamlining workflows and accelerating reimbursements. Live AI monitoring features decrease errors, flagging potential compliance issues for proactive adherence and escalation management.
Cloud-based solutions: Shifting from manual processes to secure cloud-based solutions streamlines medical billing and improves patient relationship management, making operations more scalable and positioning organizations for sustainable growth.
Constant updates, remote collaboration, and automated routine tasks remove risks of manual data-entry error, enhancing security and HIPAA compliance in medical billing outsourcing.
Advanced analytics for Revenue Cycle Management: Vital to the financial health of your organization, AI tools track performance to gather detailed insights into operations and opportunities for growth. This enables teams to predict and prevent claim denials and billing errors, track cash flow, and identify revenue leakages, resulting in better RCM and patient success.
Technology systems securely integrate with Electronic Health Record systems to boost accuracy, compliance, and speed to reimbursement. In 2026, we anticipate more detailed and nuanced insights for widespread application.
Medical billing outsourcing FAQs
What is medical billing outsourcing?
Medical billing outsourcing is when a medical provider hires external medical billing specialists to handle claim management, from coding to submission to follow-up.
How much does medical billing outsourcing cost?
Outsourced medical billing costs range from $400 to $5,000 per month depending on the service provider, campaign size and complexity, agent headcount and location, and technology implementation fees.
Is outsourcing medical billing worth it for small practices?
Yes, outsourcing medical billing can be worth the costs for small practices experiencing high volume, internal overwhelm and attrition, or compliance issues who seek specialized expertise for Revenue Cycle Management.
What are the pros and cons of outsourcing medical billing?
Pros of Outsourced Medical Billing: Dedicated experts spend all their time managing, tracking, and following up on claims. This helps prevent denials and improve speed of reimbursements, improving cash flow and compliance.
Cons of Outsourced Medical Billing: Healthcare providers give up direct control over processes. Low-quality providers can put compliance and security at risk.
How does medical billing outsourcing improve cash flow?
Outsourced medical billing improves cash flow through key strategies:
Accelerated Processes: Effective claim management is prompt and accurate, increasing the likelihood of claims being accepted on the first attempt and reducing costs of reworking claims.
Reduced Denials: Specialists focus on monitoring claims and identifying issues for prompt resolution, reducing denials.
Enhanced Accountability: Real-time updates, regular reporting, and data-driven insights prevent compliance issues and identify revenue-generating opportunities.
Is outsourced medical billing HIPAA compliant?
Not every outsourcing provider is HIPAA compliant, but high-quality medical billing providers must be HIPAA compliant, following strict data control and security protocols.
In-house vs outsourced medical billing: which is better?
In-house medical billing may be more beneficial for medical practices experiencing low demand. Outsourced medical billing is better for organizations experiencing high or fluctuating claim volumes, internal overwhelm, high operational costs, and compliance issues. Outsourcing scales operations while boosting efficiency and cash flow.
What are the latest trends in medical billing outsourcing?
The latest trend in medical billing outsourcing in 2026 is using AI technologies to improve billing and coding accuracy, track potential issues, and automate routine tasks in a secure cloud-based platform. Healthcare companies are turning to medical billing specialists to handle increasingly complex tasks for the health and long-term scalability of their practice.




